David Dowdy's research on tuberculosis overlaps with a number of different research fields, including public health, economics and epidemiology. “In this world of specialization I think it's critical also to have people who can speak multiple scientific languages,” says Dowdy, who is an assistant professor at Johns Hopkins University. “Being ‘multilingual’, so to speak, is part of what keeps my job interesting and fun, not to mention that it also enables me to interact with the most interesting people from each sphere.”

David Dowdy. Image CCBY 3.0 D. Dowdy.
After studying chemistry and biology as an undergraduate at Duke University, Dowdy did a Master’s degree in the Department of Epidemiology at Johns Hopkins. “I went to Hopkins not knowing much about public health, but I ended up doing a thesis on the diagnosis of tuberculosis in the hospital from an economic perspective,” he recalls. “As it happens I had no formal economic training either.”
Dowdy decided to stay at Johns Hopkins and enter the MD/PhD program, continuing his work on tuberculosis for his PhD dissertation. “Even though my Master’s thesis was an economic evaluation, most of my time was initially spent in the lab,” he says. “However, I gradually moved away from the lab and toward more applied endeavors.” Dowdy’s mentor for his PhD work was Dick Chaisson, an expert in tuberculosis and HIV. “Dick encouraged me to study epidemiological modeling of tuberculosis because it was a niche that Hopkins needed to fill,” he recalls.
After graduating in 2008, Dowdy completed three years as a resident in internal medicine at the University of California, San Francisco, before returning to Johns Hopkins to take up a faculty position in 2011.
So how does Dowdy feel about working mostly on interdisciplinary projects? “It's often a challenge knowing that I'm never the smartest or most knowledgeable person in any one field,” he says, “but having the chance to lead a diverse professional life is more than worth that cost to me.”
Dowdy's goal is to make models that can help epidemiologists and decision makers to select an intervention that suits a particular geographical location: the best way of diagnosing tuberculosis in New York, for example, is unlikely to also be best for rural Africa. In a recent eLife paper, Dowdy and co-workers at Massachusetts General Hospital, Sheffield University and Johns Hopkins detailed an open-source mathematical model that can predict the impact and cost of different diagnostic tests for tuberculosis. The model relies on four input parameters: the current incidence rate, the proportion of multi-drug resistant cases, the cost to treat an infected patient, and the prevalence of HIV.
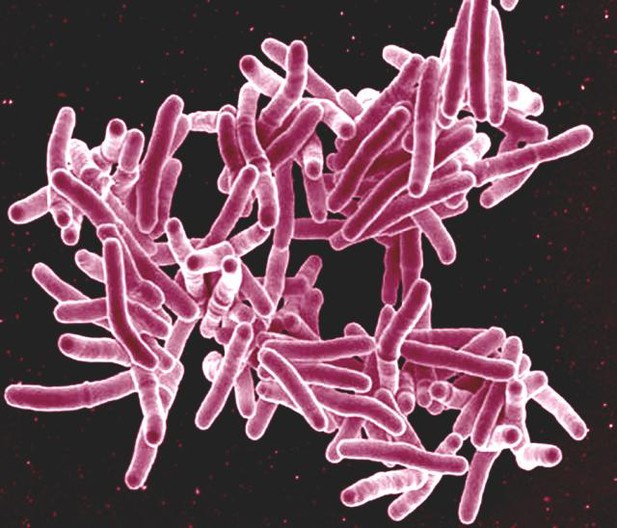
TB is caused by Mycobacterium tuberculosis. Image CCBY 2.0 NIADI.
The model does not produce one correct answer. Rather, it provides a cost-effectiveness evaluation of different diagnostic strategies under a particular set of conditions. “A test with same-day results - that is, patients get their results before they leave the clinic - would have the biggest impact,” says Dowdy, “but it would also be the costliest.” Moreover, offering such tests to large numbers of people would be a challenge in the developed world, never mind the developing world.
Dowdy continues to work on refining the model. Recently he has presented his findings to an international committee consisting of policy makers, public health officials, researchers and physicians. Their feedback is now being incorporated into a future version of the model.
“We need to think about what we can do to make the model more useful and more helpful to people,” says Dowdy. “We will work until we get to a solution where we are actually able to use these kinds of models to help not only academics publish papers but also public health officials to make real world decisions.”
David Dowdy CV
- 2013 – present: Assistant Professor, Department of Epidemiology, John Hopkins Bloomberg School of Public Health, and the Centre for Tuberculosis Research, John Hopkins University USA
- 2008 – 2011: Resident in internal medicine, University of California, San Francisco, USA
- 2003 – 2008: MD/PhD, John Hopkins Bloomberg School of Public Health USA





