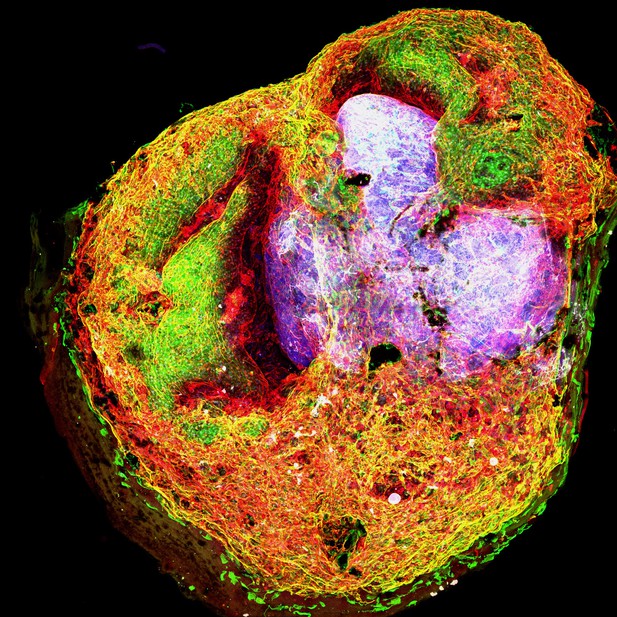
A fused organoid with blood vessels shown in green, endothelial cells shown in red, and brain cells shown in gray. Image credit: Xin-Yao Sun (CC BY 4.0)
Understanding how the organs form and how their cells behave is essential to finding the causes and treatment for developmental disorders, as well as understanding certain diseases. However, studying most organs in live animals or humans is technically difficult, expensive and invasive. To address this issue, scientists have developed models called ‘organoids’ that recapitulate the development of organs using stem cells in the lab. These models are easier to study and manipulate than the live organs.
Brain organoids have been used to recapitulate brain formation as well as developmental, degenerative and psychiatric brain conditions such as microcephaly, autism and Alzheimer’s disease. However, these brain organoids lack the vasculature (the network of blood vessels) that supplies a live brain with nutrients and regulates its development, and which has important roles in brain disorders. Partly due to this lack of blood vessels, brain organoids also do not develop a blood brain barrier, the structure that prevents certain contents of the blood, including pathogens, toxins and even certain drugs from entering the brain. These characteristics limit the utility of existing brain organoids.
To overcome these limitations, Sun, Ju et al. developed brain organoids and blood vessel organoids independently, and then fused them together to obtain vascularized brain organoids. These fusion organoids developed a robust network of blood vessels that was well integrated with the brain cells, and produced more neural cell precursors than brain organoids that had not been fused. This result is consistent with the idea that blood vessels can regulate brain development.
Analyzing the fusion organoids revealed that they contain structures similar to the blood-brain barrier, as well as microglial cells (immune cells specific to the brain). When exposed to lipopolysaccharide – a component of the cell wall of certain bacteria – these cells responded by initiating an immune response in the fusion organoids. Notably, the microglial cells were also able to engulf connections between brain cells, a process necessary for the brain to develop the correct structures and work normally.
Sun, Ju et al. have developed a new organoid system that will be of broad interest to researchers studying interactions between the brain and the circulatory system. The development of brain-blood-barrier-like structures in the fusion organoids could also facilitate the development of drugs that can cross this barrier, making it easier to treat certain conditions that affect the brain. Refining this model to allow the fusion organoids to grow for longer times in the lab, and adding blood flow to the system will be the next steps to establish this system.




