The number of women screened for both cervical and colorectal cancer in the US is far below the recommended rates for each, according to a study reported today in eLife.
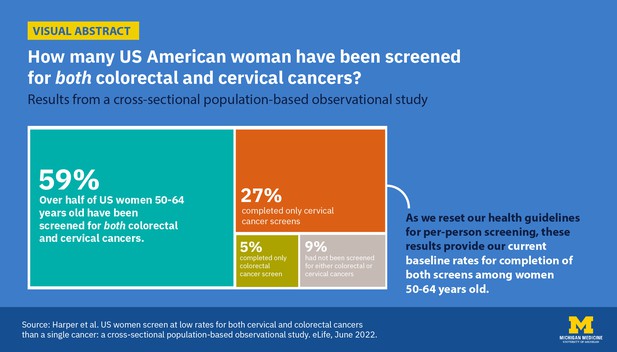
Visual representation of the percentages of colorectal and cervical cancer screening uptake among US women. Image credit: Bettina Barillas (CC BY 4.0)
The results suggest that standard reporting methods for screening uptake paint a rosier picture than reality as they focus on single cancers and not a person’s overall uptake of screening for different diseases.
“Instead of counting people with screenable cancers, national surveys count the number of cancers in the population,” explains lead author Diane Harper, Professor in the Department of Family Medicine at the University of Michigan, US. “This counting method encourages single cancer screening programs in multiple different settings, rather than a person-centric approach where screening for a range of cancers is coordinated by a primary care doctor. The harm in focusing on the single cancer screen approach is that a gap in both cervical and colorectal cancer screening has emerged for women who are least likely to screen for either cancer alone.”
Although rates of colorectal cancer screening uptake have been improving, the Center for Disease Control (CDC)’s Behavioral Risk Factor Surveillance System (BRFSS) recently showed a significant gap in uptake among women aged 50–64 years old, with self-reported rates as low as 50% for the youngest in the group. On the other hand, cervical cancer screening has been declining in the past few decades, with the lowest rates also among women aged 50–64 years old. The US national targets for cervical and colorectal cancer screening uptake separately are 84.3% and 74.4%, respectively.
This study aimed to understand the factors that predict whether women will be up to date with both colorectal and cervical cancer screening. It used data from the BRFSS, an annual US health-related telephone survey that collects state-level data about residents regarding their health-related risk behaviours and completion of services such as screening.
The researchers grouped women into four mutually exclusive categories: up to date for dual screening, each single screen, or neither screen, to determine which factors – such as age, race, education and other health conditions – were associated with completion of dual screening versus single or no screens at all.
Among women aged 50–64 years, 58.2% reported completing both colorectal and cervical cancer screening. Just 27.1% reported completing cervical cancer screening, 9.3% completed no screening and only 5.4% reported completing colorectal cancer screening. This means that women who chose only one screen chose cervical cancer screening five times more often than colorectal cancer screening.
However, when this is compared to the traditional way of reporting cancer screening (as number of cancers), the uptake looks remarkably different – 86% for cervical cancer and 64% for colorectal cancer.
Compared to women who did not screen at all, women who were most likely to be dual-screened were older, had more chronic health conditions, were more educated, had the highest incomes and were most likely to be unemployed (either a homemaker, retired or a student).
There were also racial disparities in screening uptake: Black and Hispanic women were more likely than White women to complete both screens compared to no screen. Women who identified as Asian, American Indian, or multiracial were much less likely than White women to complete colorectal cancer screening than no screen. Among all race groups, Hispanic women had the lowest uptake of both screens (46.5%) and had the highest for cervical cancer screening alone (39.4%).
“We have found that screening received by each woman shows a much lower rate of dual screening than single cancer screening rates,” concludes Harper. “A patient-centered approach that considers the total number of screens each woman has and focuses on dual screening strategies rather than single cancer screening programmes, can facilitate timely testing and the management of abnormal results. This change in focus would allow cancer screening to be incorporated into whole-person health management.”
Media contacts
Emily Packer
eLife
e.packer@elifesciences.org
+441223855373
About
eLife transforms research communication to create a future where a diverse, global community of scientists and researchers produces open and trusted results for the benefit of all. Independent, not-for-profit and supported by funders, we improve the way science is practised and shared. From the research we publish, to the tools we build, to the people we work with, we’ve earned a reputation for quality, integrity and the flexibility to bring about real change. eLife receives financial support and strategic guidance from the Howard Hughes Medical Institute, Knut and Alice Wallenberg Foundation, the Max Planck Society and Wellcome. Learn more at https://elifesciences.org/about.
To read the latest research in Medicine published in eLife, visit https://elifesciences.org/subjects/medicine.




