Repression of PRMT activities sensitize human homologous recombination-proficient ovarian and breast cancer cells to PARP inhibitor treatment
Figures
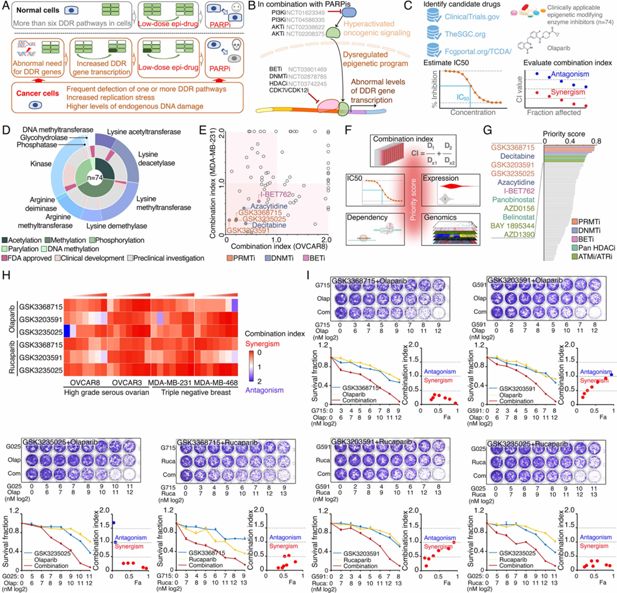
Identification of synergistic actions between PRMTis and PARPi using a drug combination screen.
(A) Illustration of the “induced PARPi sensitivity by epigenetic modulation” strategy for treatment of cancer patients with HR-proficient tumors. Due to frequent defection of one or more DDR pathways, increased replication stress, and higher endogenous DNA damage levels, cancer cells highly rely on the DDR pathways for survival compared with normal cells. During tumorigenesis, to solve these crises, certain DDR-related genes are pathologically upregulated in cancer cells. Epigenetic mechanisms represent a major strategy used by cancer cells to maintain or restore their abnormal need for DDR gene expression, resulting in a targetable vulnerability. This ‘Achilles’ heel’ can be targeted by epigenetic modulators. (B) Examples of the clinical trials based on the ‘induced PARPi sensitivity by epigenetic modulation’ strategy. The combinations of PARPis with the epi-drugs or small molecules that indirectly modulate DDR gene transcription were evaluated in the clinic. (C) Illustration of the drug combination screen approach used in this study. (D) The 74 epigenetic modifying enzyme inhibitors in the panel that was used for the drug combination screen were classified based on their mechanisms of action and target developmental levels. (E) The combination index (CI) values were generated from a drug combination screen between olaparib and each epigenetic inhibitor in OVCAR8 and MDA-MB-231 cell lines. The CI quantitatively depicts synergism (CI <0.83), additive effect (CI = 0.83–1.2), and antagonism (CI >1.2). (F) Five weighted features were collected and used to estimate the priority scores. (G) The epigenetic inhibitors were ranked based on their priority scores, and the top prioritized inhibitors are highlighted. Color indicates mechanism of action. (H) The heatmap shows average CI values between PARPis (olaparib or rucaparib) and PRMTis (GSK3368715, GSK3235025, or GSK3203591) in OVCAR8, OVCAR3, MDA-MB-231, and MDA-MB-468 cell lines. Color (red, synergism; blue, antagonism) intensity (light to dark) indicates increasing average CI values for each combination. (I) An example of the sensitivity of cancer cells to PARPi alone, PRMTi alone, and a PARPi and PRMTi combination. Only results from OVCAR8 cells are shown here. The results from other cell lines are provided in Figure 1—figure supplement 1. For each treatment, the upper panel shows crystal violet staining of a colony formation assay; the lower left panel shows a quantified survival fraction; and the lower right panel shows the CI values. Fa, fraction affected.

The sensitivity of cancer cells to PARPi alone, PRMTi alone, and a PARPi and PRMTi combination in a panel of HGSOC and TNBC cell lines.
For each treatment, the upper panel shows crystal violet staining of a colony formation assay; the lower left panel shows a quantified survival fraction; and the lower right panel shows the CI values. Fa, fraction affected.
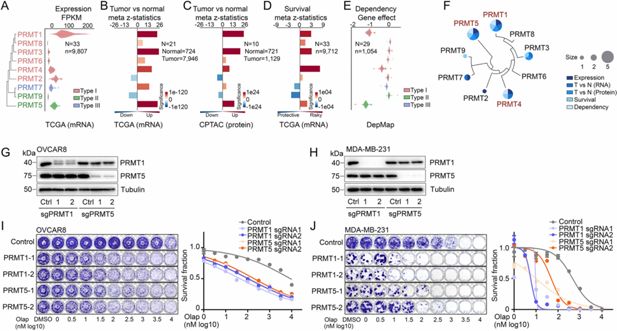
PRMT1, PRMT4/CARM1, and PRMT5 are potential therapeutic targets in oncology.
(A) mRNA expression levels of the PRMT family across the TCGA tumor samples. Each spot represents the average mRNA expression level of a cancer type (n=33). (B and C) Meta z-statistics of mRNA (B) and protein (C) expression levels of the PRMT family in tumors compared with corresponding controls in the TCGA (B) or CPTAC (C) cohorts. Red and blue indicate up- and down-regulation, respectively. (D) Meta z-statistics of the association between mRNA expression and patient outcome for the PRMT family across the TCGA cohort. Red and blue indicate poor and good outcomes, respectively. (E) The dependency effects of the PRMT family based on the CRISPR screen from the DepMap project. Each spot represents the average gene effect of a cancer type (n=29). A lower effect score indicates that a gene is more likely to be dependent in cancer cells. (F) Summary of the above five features for each gene in the PRMT family. (G and H) Western blot analyses of PRMT1 and PRMT5 expression in OVCAR8 (G) and MDA-MB-231 (H) cells in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9. (I and J) Sensitivity of olaparib in OVCAR8 (I) or MDA-MB-231 (J) cells in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9. Left panel: crystal violet staining of a colony formation assay; right panel: survival fraction quantified from the left panel.
-
Figure 2—source data 1
PDF file containing original western blots for Figure 2G and H, indicating the relevant bands.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig2-data1-v1.pdf
-
Figure 2—source data 2
Original file for western blots displayed in Figure 2G and H.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig2-data2-v1.zip

Expression levels of the PRMTs across the TCGA tumor specimens.
(A) The heatmap of mRNA expression levels of PRMT family across the TCGA tumor samples. The intensity of heatmap color indicates the FPKM value for each percentile (25th, 50th, 75th, and 90th) of an individual PRMT gene in a given cancer type. (B) The mRNA expression levels of the PRMT family in tumors compared with corresponding controls in the TCGA cohorts. Red and blue indicate up- and down-regulation, respectively. (C) The protein expression levels of the PRMT family in tumors compared with corresponding controls in the CPTAC cohorts. Red and blue indicate up- and down-regulation, respectively.
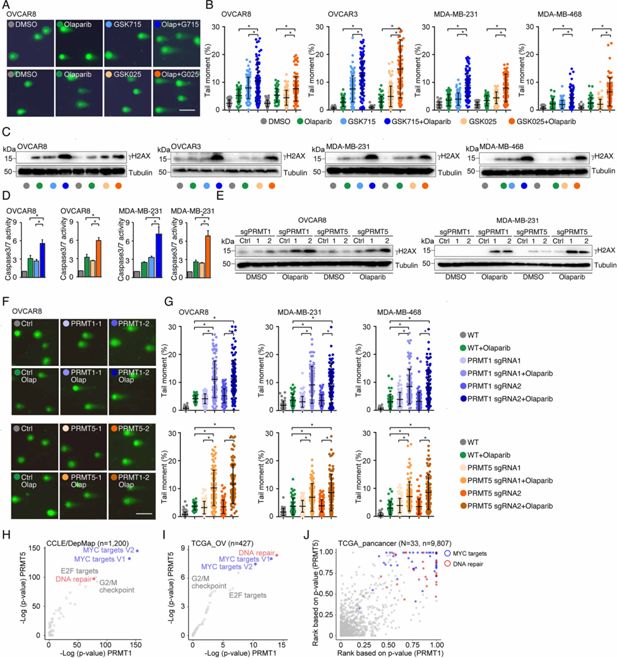
PRMT inhibition enhances PARPi treatment-induced DNA damage in cancer cells.
(A) A comet assay was used to measure DNA damage in cancer cells treated with DMSO, olaparib (5 μM, 96 hr), GSK3368715 (5 μM, 96 hr), GSK3235025 (5 μM, 96 hr), or combinations (representative images from OVCAR8). Scale bars, 10 μm. (B) The extent of DNA damage was quantified using the tail moment in comet assays of OVCAR8, OVCAR3, MDA-MB-231, and MDA-MB-468 cell lines treated with DMSO, olaparib, GSK3368715, GSK3235025, or combinations. Data are presented as means ± SDs, *p<0.05 determined by two-tailed Student’s t tests. (C) Western blot analyses of γH2AX in cancer cells treated with DMSO, olaparib, GSK3368715, GSK3235025, or combinations. (D) Caspase-3/7 activity was measured using a caspase-Glo 3/7 assay in OVCAR8 and MDA-MB-231 cells treated with DMSO, olaparib, GSK3368715, GSK3235025, or combinations. Data are presented as means ± SDs, n=3 biological replicates, *p<0.05 determined by two-tailed Student’s t tests. (E) Western blot analyses of γH2AX in OVCAR8 and MDA-MB-231 cells in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9. (F) A comet assay was used to measure olaparib treatment-induced DNA damage in cells in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9 (representative images from OVCAR8). Scale bars, 10 μm. (G) The extent of olaparib treatment-induced DNA damage was quantified using the tail moment in comet assays of OVCAR8, MDA-MB-231, and MDA-MB-468 cell lines in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9. Data are presented as means ± SDs, *p<0.05 determined by two-tailed Student’s t tests. (H) and (I) Correlations between the expression levels of PRMT1/PRMT5 and ‘50 hallmark’ molecular signatures in the cancer cell lines from the DepMap (H) and primary tumor specimens from the TCGA (ovarian cancer was represented as an example, I) cohort. (J) Correlations between the expression levels of PRMT1/PRMT5 and ‘50 hallmark’ molecular signatures across primary tumor specimens from the TCGA cohort. For each cancer type, the correlations between PRMT1/5 expression and ‘50 hallmark’ molecular signatures were ranked 0–1 based on the p-values, with 1 indicating the most significant signature. Red and blue circles indicate DNA repair and Myc signatures, respectively.
-
Figure 3—source data 1
PDF file containing original western blots for Figure 3C and E, indicating the relevant bands and treatments.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig3-data1-v1.pdf
-
Figure 3—source data 2
Original file for western blots displayed in Figure 3C and E.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig3-data2-v1.zip

Comet assay was used to measure DNA damage in cancer cell lines in which PRMTs were inhibited by chemical compounds or genetic approach.
(A) Left panels: A comet assay was used to measure DNA damage in OVCAR8, OVCAR3, MDA-MB-231, and MDA-MB-468 cell lines treated with DMSO, olaparib, GSK3368715, GSK3235025, or combinations. Scale bars, 10 μm. Right panels: The extent of DNA damage was quantified using the tail moment in comet assays of OVCAR8, OVCAR3, MDA-MB-231, and MDA-MB-468 cell lines treated with DMSO, olaparib, GSK3368715, GSK3235025, or combinations. Data are presented as means ± SDs, *p<0.05 determined by two-tailed Student’s t tests. (B) Left panels: A comet assay was used to measure olaparib treatment-induced DNA damage in OVCAR8, MDA-MB-231, and MDA-MB-468 cell lines in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9. Scale bars, 10 μm. Right panels: The extent of olaparib treatment-induced DNA damage was quantified using the tail moment in comet assays of OVCAR8, MDA-MB-231, and MDA-MB-468 cell lines in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9. Data are presented as means ± SDs, *p<0.05 determined by two-tailed Student’s t tests.
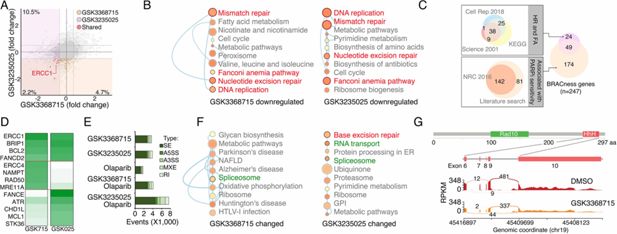
PRMTis maintain the expression of genes associated with DNA damage repair (DDR) and BRCAness.
(A) The dot plot shows the gene expression changes measured by RNA-seq in MDA-MB-231 cells. The BRCAness genes that were repressed by GSK3368715 and GSK3235025 treatments are highlighted with color. (B) The top 10 KEGG pathways in which genes downregulated by GSK3368715 (left) and GSK3235025 (right) treatments were significantly enriched. Circle size indicates the fold enrichment. Lines indicate numbers of shared genes between pathways. The DDR pathways are highlighted in red. (C) Illustration BRCAness gene collection method. First, the genes in two major DDR pathways associated with PARPi sensitivity (HR and FA) were collected from three independent databases. In total, 73 genes annotated by at least two databases were defined as HR/FA genes. Second, the genes associated with PARPi sensitivity were retrieved from a Nature Reviews paper (n=142). An additional 81 genes were identified through a manual literature search using PubMed. In total, 223 genes were defined as PARPi sensitivity-associated genes. Taken together, 247 genes were defined as ‘BRCAness genes’ in this study. (D) The heatmap shows qRT-PCR validation of a group of BRCAness genes. Green color intensity indicates fold changes. (E) The abnormal splicing event numbers induced by different treatments compared with the control treatment (DMSO) in MDA-MB-231 cells. Types of abnormal splicing events are indicated by different colors. (F) The top 10 KEGG pathways in which abnormally spliced genes after GSK3368715 (left) and GSK3235025 (right) treatments were significantly enriched. Circle size indicates the fold enrichment. Lines indicate numbers of shared genes between two pathways. (G) An abnormal splicing gene (ERCC1). Upper panel: the structure of ERCC1. The alternative splicing event was identified in exons 6–10, which encodes the helix-hairpin-helix (HhH) domain of ERCC1. Lower panel: Sashimi plots showing the exon truncation events of ERCC1 as detected by RNA-seq in MAD-MB-231 cells treated with DMSO and GSK3368715 independently. The X-axes indicate genomic locations, and the Y-axes indicate RNA-seq coverage. The numbers of junction reads are shown in the splice junctions (curved lines).
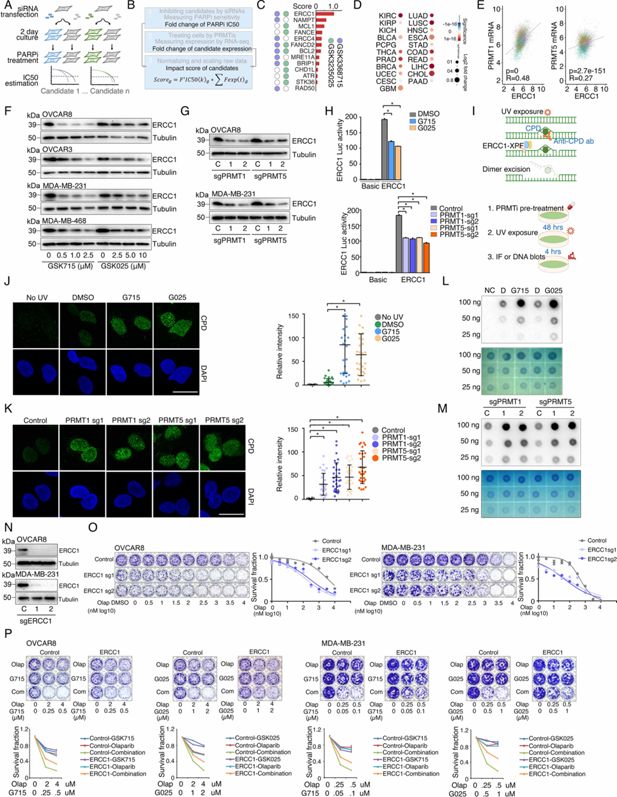
ERCC1 repression is a common mechanism by which PRMTis sensitize cells to PARPi treatment.
(A) A siRNA screen was performed to evaluate the effects of knocking down the candidate genes on PARPi sensitivity in MDA-MB-231 cells. Gray: control siRNA transfection. (B) Schematic of the impact score estimation for each candidate gene based on RNA-seq and a siRNA screen. (C) Summary of the impact scores of 13 examined candidates. (D) Expressional differences in ERCC1 mRNA levels between tumor specimens and their corresponding controls. Red and blue indicate up- and down-regulation, respectively. Size: fold change, intensity: p-value. (E) Correlations of mRNA expression levels between ERCC1 and PRMT1 (left) and PRMT5 (right) across all the TCGA tumors. Color indicates cancer type. (F) Western blot analysis of ERCC1 protein expression in cancer cells treated with different GSK3368715 and GSK3235025 concentrations, independently, for 72 hr. (G) Western blot analysis of ERCC1 protein expression in OVCAR8 and MDA-MB-231 cells in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9. (H) Luciferase reporter assay of ERCC1 core promoter activity in HEK293T cells treated with GSK3368715 (5 μM, 48 hr) and GSK3235025 (5 μM, 48 hr) independently (upper panel), or after knocking out PRMT1 and PRMT5, independently (lower panel). Statistical difference was assessed using Student’s t test, *p<0.05; n=3. Error bars represent means ± SDs. (I) Schematic of UV-induced cyclobutane pyrimidine dimers (CPD) detection by antibody (upper panel) and the experimental schedule (lower panel). (J) Representative images (left) and quantitative results (right) of UV-induced CPD formation in MDA-MB-231 cells treated independently with DMSO, GSK3368715 (2.5 μM, 96 hr), and GSK3235025 (5 μM, 96 hr). Cells not subjected to UV treatment were used as the negative control. Scale bars, 10 μm. Statistical analysis by Student’s t test, *p<0.05; n=3. Error bars represent means ± SD. (K) Representative images (left) and quantitative results (right) of UV-induced CPD formation in MDA-MB-231 cells in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9. Scale bars, 10 μm. Statistical differences were assessed using Student’s t test, *p<0.05; n=3. Error bars represent means ± SDs. (L) Dot blots of CPD levels in MDA-MB-231 cells treated independently with DMSO, GSK3368715 (5 μM, 96 hr), and GSK3235025 (5 μM, 96 hr). Cells not subjected to UV treatment were used as the negative control. Methylene blue staining was used as the loading control. (M) Dot blots of CPD levels in MDA-MB-231 cells in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9. Methylene blue staining was used as the loading control. (N) Western blot analysis of ERCC1 protein expression in OVCAR8 and MDA-MB-231 cells in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9. (O) Sensitivity of OVCAR8 and MDA-MB-231 cells to olaparib. Left panel: crystal violet staining of a colony formation assay; right panel: survival fraction quantified from the upper panel. (P) Sensitivity of OVCAR8 and MDA-MB-231 cells, which overexpressed ERCC1 owing to a lentiviral infection, to olaparib, GSK3368715, GSK3235025, and combinations. Upper panel: crystal violet staining of a colony formation assay; lower panel: the survival fraction quantified from the upper panel.
-
Figure 5—source data 1
PDF file containing original western blots for Figure 5F, G and N, indicating the relevant bands and treatments.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig5-data1-v1.pdf
-
Figure 5—source data 2
Original file for western blots displayed in Figure 5F, G and N.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig5-data2-v1.zip

Repression of ERCC1 is a common mechanism by which PRMTis sensitize cells to PARPi treatment.
(A) The expression levels of aDMA and sDMA in cancer cell lines in which PRMTs were inhibited by chemical compounds. The expression levels of aDMA and sDMA in cancer in OVCAR8, OVCAR3, MDA-MB-231, and MDA-MB-468 cell lines treated with GSK3368715 or GSK3235025. To ensure identical experimental conditions, the protein samples analyzed in these western blots were identical to those used in Figure 5F; accordingly, the same loading controls are presented in both figures. (B) The expression levels of aDMA and sDMA in cancer cell lines in which PRMTs were inhibited by genetic approach. The expression levels of aDMA and sDMA in cancer in OVCAR8 and MDA-MB-231 cell lines in which PRMT1 or PRMT5 was knocked out by CRISPR/Cas9. To ensure identical experimental conditions, the protein samples analyzed in these western blots were identical to those used in Figure 5G; accordingly, the same loading controls are presented in both figures. (C) Dot blots of CPD levels in MDA-MB-231 cells in which ERCC1 was knocked out using lentiviral CRISPR/Cas9. Methylene blue staining was used as the loading control.
-
Figure 5—figure supplement 1—source data 1
PDF file containing original western blots for Figure 5—figure supplement 1A and B, indicating the relevant bands and treatments.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig5-figsupp1-data1-v1.pdf
-
Figure 5—figure supplement 1—source data 2
Original file for western blots displayed in Figure 5—figure supplement 1A and B.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig5-figsupp1-data2-v1.zip

PRMT inhibition activates intrinsic innate immune pathways in cancer cells.
(A) The top 10 KEGG pathways in which genes upregulated by GSK3368715 (left) and GSK3235025 (right) treatments were significantly enriched. Circle size indicates fold enrichment. Lines indicate numbers of shared genes between pathways. The immune-related pathways are highlighted in red. (B) Mosaic plots show percentages of genes upregulated by GSK3368715 (upper) and GSK3235025 (lower) treatments. Right: immune-related genes, left: non-immune-related genes. Significantly more immune-related genes, compared with non-immune-related genes, were upregulated by PRMT inhibition (GSK3368715: 17.8% vs 9.4%; GSK3235025: 23.6% vs 9.9%). (C) Word cloud revealing the common immune-related genes upregulated by GSK3368715 and GSK3235025 treatments. 37.7% are associated with innate immune responses (dark red). Text size indicates meta-fold changes by both PRMTis. (D) Scaled Venn diagram showing the functional families among the common upregulated immune-related genes. (E) Western blot analysis of p-TBK1 expression in OVCAR8 (upper panel) and MDA-MB-231 (lower panel) cells treated with DMSO, olaparib (5 μM), GSK3368715 (OVCAR8, 5 μM and MDA-MB-231, 2.5 μM), GSK3235025 (5 μM) or olaparib (5 μM) combined independently with GSK3368715 (OVCAR8, 5 μM and MDA-MB-231, 2.5 μM) and GSK3235025 (5 μM) for 96 hr. (F) Western blot analysis of p-TBK1 expression in OVCAR8 (upper panel) and MDA-MB-231 (lower panel) cells in which PRMT1 and PRMT5 were independently knocked out using lentiviral CRISPR/Cas9. The cells were treated with olaparib (5 μM, 96 hr) or DMSO. (G) Representative cytoplasmic micronuclei stained by PicoGreen in OVCAR8 (upper panel) and MDA-MB-231 (lower panel) cells treated with DMSO, olaparib (5 μM), GSK3368715 (OVCAR8, 5 μM and MDA-MB-231, 2.5 μM), GSK3235025 (5 μM), and olaparib (5 μM) combined independently with GSK3368715 (OVCAR8, 5 μM and MDA-MB-231, 2.5 μM) and GSK3235025 (5 μM). White arrows: micronuclei. Scale bar: 10 μm. (H) Quantification of micronuclei from G. Micronuclei number per cell was normalized to DMSO. Statistical significance was assessed using a two-tailed Student’s t test. Error bars represent means ± SDs.
-
Figure 5—figure supplement 2—source data 1
PDF file containing original western blots for Figure 5—figure supplement 2E and F, indicating the relevant bands and treatments.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig5-figsupp2-data1-v1.pdf
-
Figure 5—figure supplement 2—source data 2
Original file for western blots displayed in Figure 5—figure supplement 2E and F.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig5-figsupp2-data2-v1.zip
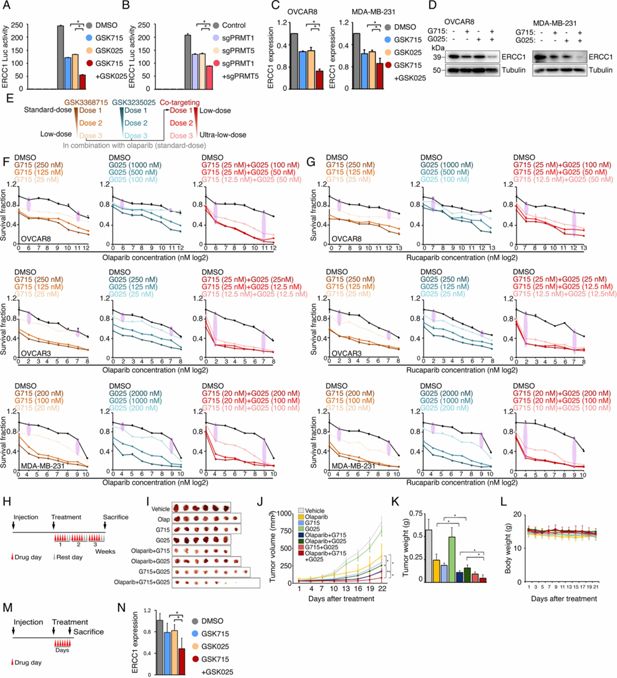
Type I PRMT and PRMT5 inhibition acts synergistically to enhance PARPi sensitivity.
(A) Luciferase reporter assay of the ERCC1 core promoter activity levels in HEK293T cells treated with DMSO, GSK3368715 (5 μM, 48 hr), and GSK3235025 (5 μM, 48 hr) independently, or with the combination of GSK3368715 (5 μM, 48 hr) and GSK3235025 (5 μM, 48 hr). Statistical differences were assessed using Student’s t test, *p<0.05; n=3. Error bars represent means ± SDs. (B) Luciferase reporter assay of the ERCC1 core promoter activity levels in HEK293T cells in which PRMT1, PRMT5, and PRMT1/5 were independently knocked out using lentiviral CRISPR/Cas9. Statistical differences were assessed using Student’s t test, *p<0.05; n=3. Error bars represent means ± SDs. (C) qRT-PCR analysis of ERCC1 RNA expression in OVCAR8 and MDA-MB-231 cells treated with GSK3368715 (5 μM) and GSK3235025 (5 μM) independently for 48 hr. (D) Western blot analysis of ERCC1 protein expression in OVCAR8 and MDA-MB-231 cells treated with GSK3368715 (5 μM) and GSK3235025 (5 μM) independently for 72 hr. (E) Dose de-escalation scheme. The lowest doses of GSK3368715 and GSK3235025 independently for PRMTi and the PARPi combination were first identified. They were then used as initial doses for triple combination. The doses of GSK3368715 and GSK3235025 were further reduced until the lowest doses for each PRMTi in the triple combination were identified. (F) Sensitivity levels of OVCAR8 (upper panel), OVCAR3 (middle panel), and MDA-MB-231 (lower panel) cells to olaparib alone or olaparib combined with three different doses of GSK3368715 (left panel), GSK3235025 (middle panel), and GSK3368715 plus GSK3235025 (right panel). (G) Sensitivity levels of OVCAR8 (upper panel), OVCAR3 (middle panel), and MDA-MB-231 (lower panel) cells to rucaparib alone or rucaparib combined with three different doses of GSK3368715 (left panel), GSK3235025 (middle panel), and GSK3368715 plus GSK3235025 (right panel). (H) Schematic of the MDA-MB-231 xenograft experimental design. MDA-MB-231 cells were implanted subcutaneously in immunodeficient nude mice and grown until tumors reached a size of approximately 30 mm3. Tumor-bearing mice were randomized and then received vehicle, 50 mg/kg olaparib i.p., 25 mg/kg GSK3368715 p.o., 50 mg/kg GSK3235025 p.o., or combinations of two agents or three agents, 5 days a week for 3 weeks. Caliper measurements were taken every other day from the initiation of drug treatment. (I) Images of tumors collected from animals receiving vehicle, olaparib, GSK3368715, GSK3235025, and combinations of two agents or three agents. (J) Tumor growth curve for each treatment group in immunodeficient nude mice. Statistical significance was assessed using a two-tailed Student’s t test. Error bars represent means ± SDs. (K) Bar plot showing the mean tumor volume of each treatment group. Statistical significance was assessed using a two-tailed Student’s t test. Error bars represent means ± SDs. (L) Changes in the body weights of different murine treatment groups. Statistical significance was assessed using a two-tailed Student’s t test. Error bars represent means ± SDs. (M) Schematic of the MDA-MB-231 xenograft experimental design. MDA-MB-231 cells were implanted subcutaneously in immunodeficient nude mice and grown until tumors reached a size of approximately 200 mm3. Tumor-bearing mice were randomized and then received vehicle, 25 mg/kg GSK3368715 p.o., 50 mg/kg GSK3235025 p.o., or combination of two agents, for 1 week. (N) qRT-PCR analysis of ERCC1 RNA expression in MDA-MB-231 xenograft tumors following 1 week of treatment.
-
Figure 6—source data 1
PDF file containing original western blots for Figure 6D, indicating the relevant bands and treatments.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig6-data1-v1.pdf
-
Figure 6—source data 2
Original file for western blots displayed in Figure 6D.
- https://cdn.elifesciences.org/articles/99225/elife-99225-fig6-data2-v1.zip
Tables
| Reagent type (species) or resource | Designation | Source or reference | Identifiers | Additional information |
|---|---|---|---|---|
| Cell line (Homo sapiens) | OVCAR8 | NCI-DTP | NCI-60 human cancer cell line panel; RRID:CVCL_1629 | |
| Cell line (Homo sapiens) | OVCAR3 | ATCC | Cat: #HTB-161; RRID:CVCL_DH37 | |
| Cell line (Homo sapiens) | MDA-MB-231 | ATCC | Cat: #CRM-HTB-26; RRID:CVCL_0062 | |
| Cell line (Homo sapiens) | MDA-MB-468 | ATCC | Cat: #HTB-132; RRID:CVCL_0419 | |
| Cell line (Homo sapiens) | HEK293T | ATCC | Cat: #CRL-3216; RRID:CVCL_0063 | |
| Antibody | Anti-PRMT1 (Rabbit polyclonal) | Cell Signaling Technology | Cat: #2449 S; RRID:AB_2237696 | WB (1:1000) |
| Antibody | Anti-PRMT5 (Rabbit monoclonal) | Cell Signaling Technology | Clone:D5P2T; Cat: #79998 S; RRID:AB_2799945 | WB (1:1000) |
| Antibody | Anti-aDMA (Rabbit monoclonal) | Cell Signaling Technology | Cat: #13522 S; RRID:AB_2665370 | WB (1:1000) |
| Antibody | Anti-sDMA (Rabbit monoclonal) | Cell Signaling Technology | Cat: #13222 S; RRID:AB_2714013 | WB (1:1000) |
| Antibody | Anti-ERCC1 (Rabbit polyclonal) | Cell Signaling Technology | Cat: #3885 S; RRID:AB_2100142 | WB (1:1000) |
| Antibody | Anti-phospho-H2AX (S139) (Mouse monoclonal) | Sigma-Aldrich | Clone:JBW301; Cat: #05–636; RRID:AB_309864 | WB (1:1000) |
| Antibody | Anti-phospho-TBK1/NAK (Rabbit monoclonal) | Cell Signaling Technology | Clone:D52C2; Cat: #5483 S; RRID:AB_10693472 | WB (1:1000) |
| Antibody | Anti-β-Tubulin (Rabbit monoclonal) | Cell Signaling Technology | Clone:9 F3 Cat: #2128; RRID:AB_823664 | WB (1:1000) |
| Antibody | Anti-Cyclobutane Pyrimidine Dimers (CPDs) (Mouse monoclonal) | Cosmo Bio | Clone:TDM-2; Cat: #CAC-NM-DND-001; RRID:AB_1962813 | IF (1:1000) |
| Recombinant DNA reagent | LentiCRISPRv2 (plasmid) | Addgene | Cat:#98290 | |
| Recombinant DNA reagent | LentiCRISPRv2-PRMT1-sgRNA1 (plasmid) | This paper | PRMT1 targeting CRISPR plasmid; Guide:GTGGATGCCAAAGTGTGCGT | |
| Recombinant DNA reagent | LentiCRISPRv2-PRMT1-sgRNA2 (plasmid) | This paper | PRMT1 targeting CRISPR plasmid; Guide:CCTTGGCAGCAAACATGCAG | |
| Recombinant DNA reagent | LentiCRISPRv2- PRMT5-sgRNA1 (plasmid) | This paper | PRMT5 targeting CRISPR plasmid; Guide:ATGAACTCCCTCTTGAAACG | |
| Recombinant DNA reagent | LentiCRISPRv2- PRMT5-sgRNA2 (plasmid) | This paper | PRMT5 targeting CRISPR plasmid; Guide:GATTCGTCCAGACTCAAAAG | |
| Recombinant DNA reagent | LentiCRISPRv2- ERCC1-sgRNA1 (plasmid) | This paper | ERCC1 targeting CRISPR plasmid; Guide:ATTTGTGATACCCCTCGACG | |
| Recombinant DNA reagent | LentiCRISPRv2- ERCC1-sgRNA2 (plasmid) | This paper | ERCC1 targeting CRISPR plasmid; Guide:ATATTCGGCGTAGGTCTGAG | |
| Recombinant DNA reagent | CD513B (plasmid) | System Biosciences | Cat: #CD513B | |
| Recombinant DNA reagent | CD513B-human ERCC1 (plasmid) | This paper | ERCC1 over-expression in CD513B | |
| Recombinant DNA reagent | pGL3 Basic Vector (plasmid) | Addgene | Cat: #212936 | |
| Recombinant DNA reagent | pGL3 Basic-ERCC1 promoter Vector (plasmid) | This paper | ERCC1 promoter version of pGL3 Basic | |
| Commercial assay or kit | Dual-Luciferase Reporter Assay System | Promega | Cat: #E1910 | |
| Chemical compound, drug | Crystal violet | Millipore Sigma | Cat: #32675 | Colony formation assay (0.5%) |
| Chemical compound, drug | SYBR Gold Nucleic Acid Gel Stain | Thermo Fisher Scientific | Cat: #S11494 | Comet assay (1:10,000) |
| Chemical compound, drug | PicoGreen | Thermo Fisher Scientific | Cat: #P11496 | IF (1:1000) |
| Chemical compound, drug | FuGENE 6 Transfection Reagent | Promega | Cat: #E2691 |
Additional files
-
Supplementary file 1
Supplementary tables A to J.
(A) List of the epigenetic modulators that were used in initial drug combination screen. (B) List of the specimens that were used in this study from the TCGA project. (C) Expression of the PRMTs across cancers. (D) Recurrent genomic alterations of the PRMTs across cancers. (E) Cell dependencies of PRMTs from the DepMap project. (F) Correlations between the expression levels of PRMT1/5 and “50 hallmark” molecular signatures across the TCGA tumor specimens. (G) List of the potential BRCAness genes in the human genome. (H) List of the BRCAness genes that were repressed by PRMTi treatment. (I) PRMTi and PARPi combination concentration in each cancer line. (J) Primers and oligoes that were used in this study.
- https://cdn.elifesciences.org/articles/99225/elife-99225-supp1-v1.xlsx
-
MDAR checklist
- https://cdn.elifesciences.org/articles/99225/elife-99225-mdarchecklist1-v1.docx






